4 Cancer Breakthroughs that Give Us Hope
These four recent developments are all science, no hype.
By Juno DeMelo
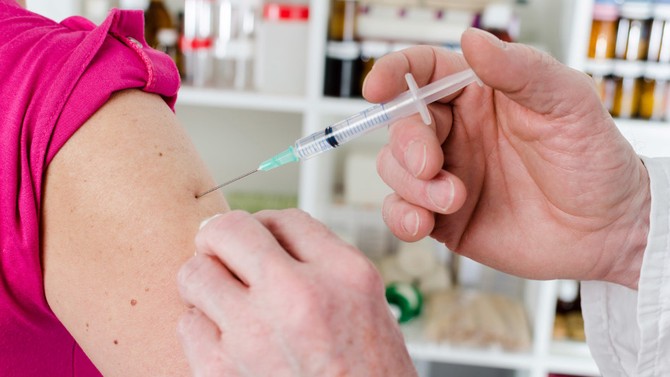
Photo: thodonal/istock
More than 1.6 million new cancer cases are expected to be diagnosed this year—on top of the 14.5 million people already living with the disease. Now for the good news: Death rates are falling for the four most common cancer types (lung, colorectal, breast and prostate), and researchers are ever closer to extending survival rates and possibly even finding cures. The advances that should be on your radar:
Immunity-Boosting Injections
One reason it's so hard to treat cancer: Malignancies can go undetected by the T cells that help our bodies fight disease. But a new type of treatment, chimeric antigen receptor (CAR) T-cell therapy, genetically modifies patients' T cells so they can recognize cancer—and get to work. "We've figured out how to identify proteins on a tumor cell that are more pronounced than you would see in normal tissue, then program the T cells to target those proteins," explains Behnam Badie, MD, chief of neurosurgery at City of Hope, a research and treatment center for cancer and other life-threatening diseases—and the first center in the U.S. to inject CAR T cells directly into brain tumors. "We already know this therapy works in the lab," Badie says. "We're now testing it on patients with brain tumors that haven't responded to radiation, surgery, or chemotherapy."
Immunity-Boosting Injections
One reason it's so hard to treat cancer: Malignancies can go undetected by the T cells that help our bodies fight disease. But a new type of treatment, chimeric antigen receptor (CAR) T-cell therapy, genetically modifies patients' T cells so they can recognize cancer—and get to work. "We've figured out how to identify proteins on a tumor cell that are more pronounced than you would see in normal tissue, then program the T cells to target those proteins," explains Behnam Badie, MD, chief of neurosurgery at City of Hope, a research and treatment center for cancer and other life-threatening diseases—and the first center in the U.S. to inject CAR T cells directly into brain tumors. "We already know this therapy works in the lab," Badie says. "We're now testing it on patients with brain tumors that haven't responded to radiation, surgery, or chemotherapy."

Illustration: Chris Silas Neal
Cancer That Kills Cancer
Most cancer treatments come with serious side effects. "You're trying to kill one cell in a neighborhood of other cells that are chemically similar, and the collateral damage is terrible," says Richard Lerner, MD, a professor of immunochemistry at the Scripps Research Institute in San Diego. "The holy grail would be not to kill cancer cells but to turn them into something else." Lerner's team found that by applying antibodies to leukemia cells in their lab, they could convert them into immature dendritic cells, which support the body's immune system. Even more amazing, they found that these new cells actually turned into natural killer cells, wiping out up to 16 percent of the surrounding leukemia cells—and only leukemia cells—within 24 hours.
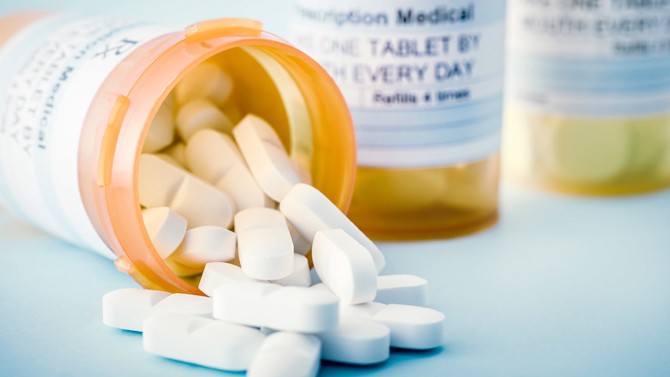
Photo: Sezeryadigar/iStock
Cancer-Fighting Heart Meds
Beta-blockers have long been used to lower blood pressure; soon they may also extend the lives of women with ovarian cancer, which is responsible for more deaths than any other female reproductive system cancer. A recent study found that patients with ovarian-related cancers who took beta-blockers during chemo survived an average of 47 months versus 42 for those who didn't use them. And those taking a specific version that targets multiple beta-receptors had a median survival of about 95 months. "Beta-blockers dampen the effects of stress hormones, which fuel the progression of cancer," explains principal investigator Anil Sood, MD, a professor of gynecologic oncology at the University of Texas MD Anderson Cancer Center. While it's too early to recommend heart meds for ovarian cancer patients, "the drugs could be ready for prime time if they continue to show promise," says Sood.

Photo: OJO_Images/istock
Venture Capital for Cancer Research
One in eight women will develop breast cancer in her lifetime, and in a significant number of cases, that cancer will metastasize. But research into how and why cancer spreads has lagged—until now, says Larry Norton, MD, scientific director of the Breast Cancer Research Foundation and deputy physician in chief for breast cancer programs at Memorial Sloan Kettering in New York City. Norton is helping direct Aurora, a three-year-old initiative that's disbursing $31 million to scientists around the world to study the molecular basis of metastases. "The way science has approached breast cancer is to figure out why the cows are in the field by studying the ones who stayed in the barn," says Norton. "We're looking at metastatic specimens—the field cows—to learn why cells spread; if we can stop them from spreading, tumors would be nothing worse than pimples. For people with metastatic cancer, there's real hope, and this major effort is finding it."
From the May 2016 issue of O, The Oprah Magazine

