Taking Control

For five years, former CBS anchorwoman René Syler suffered through abnormal mammograms and painful biopsies—until she decided to take control of her health. Both René's mother and father had been diagnosed with breast cancer, and she knew she could be next.
"Whenever a doctor finds out that your father had breast cancer, it's an immediate red flag, because men without a lot of estrogen should not be having breast cancer," René says.
With such a strong family history, René's risk factor was a concern for doctors. Then, five years ago her mammogram started showing signs of abnormality. "Every year I would go in, and every year it was the same thing. A mammogram followed by a biopsy, followed by three days of [wondering] if I have cancer."
At first, René underwent stereotactic biopsies, which use needles to remove the tissue. Then, the tests started to get more involved. "They would take out breast tissue that's roughly the size of a golf ball. And the last time, they had to take out three such areas in the left breast," René says.
"Whenever a doctor finds out that your father had breast cancer, it's an immediate red flag, because men without a lot of estrogen should not be having breast cancer," René says.
With such a strong family history, René's risk factor was a concern for doctors. Then, five years ago her mammogram started showing signs of abnormality. "Every year I would go in, and every year it was the same thing. A mammogram followed by a biopsy, followed by three days of [wondering] if I have cancer."
At first, René underwent stereotactic biopsies, which use needles to remove the tissue. Then, the tests started to get more involved. "They would take out breast tissue that's roughly the size of a golf ball. And the last time, they had to take out three such areas in the left breast," René says.

After recovering from her last lumpectomy in July 2006, René was stunned by what she saw—her left breast was about a half cup size smaller than her right. "I cried. It was sad, because I felt like I'm a young woman and I worked hard to keep my figure and my shape, and I didn't want to feel like I was deformed," she says.
Her relief at being assured that she was cancer-free after each of her four biopsies soon evaporated into another year of worry. "I lived with this fear that the other shoe was going to drop after every mammogram and every biopsy," she says.
Her relief at being assured that she was cancer-free after each of her four biopsies soon evaporated into another year of worry. "I lived with this fear that the other shoe was going to drop after every mammogram and every biopsy," she says.

Despite all the testing—including MRIs and sonograms—the threat of breast cancer still loomed. "I had this sort of moment where I thought, 'What am I doing?'" René says. "Am I waiting for the day or the year that they finally say, 'Well now you do have breast cancer?' Is that what I'm waiting for?"
René began to look at her options, considering every possible angle with the help of her doctor and a psycho-oncologist. Armed with as much information as possible, René made the decision she felt was right for her—a prophylactic mastectomy.
"I'd been thinking about this for probably two years. This is not a decision that was made overnight or in a vacuum," she says.
Still, René's decision was an emotional one. In the end, she knew she had to do what was right for her children. "I felt like it was important for me to be there for my family, even if a part of me was missing," she says.
René began to look at her options, considering every possible angle with the help of her doctor and a psycho-oncologist. Armed with as much information as possible, René made the decision she felt was right for her—a prophylactic mastectomy.
"I'd been thinking about this for probably two years. This is not a decision that was made overnight or in a vacuum," she says.
Still, René's decision was an emotional one. In the end, she knew she had to do what was right for her children. "I felt like it was important for me to be there for my family, even if a part of me was missing," she says.

René allowed Oprah's cameras to document the days leading up to her double mastectomy. The night before her surgery, René admitted that she felt emotionally drained…and a little nervous.
Before leaving for the hospital the next morning, René wrote notes to her children, Cole and Casey, and assured them that she would be okay…but even she didn't know what to expect.
"I have no idea what tomorrow morning's going to be like," she said on the way to the hospital. "I would like to think that there's going to be this immediate sense of relief, in terms of I don't have to worry about ever being diagnosed with breast cancer."
What she did know was that she couldn't continue to live in fear. "My gut tells me I've had enough," she said. "I can't keep doing this to my family. I can't keep doing this to myself."
After René and her husband, Buff, arrived at Memorial Sloan-Kettering Cancer Center in New York City, reality set in. One hour before surgery, René's emotions came pouring out. Through her tears, she asked Buff if she was making the right decision. "I was fine until [the doctor] said we were ready to go to surgery, and then I got scared," she said. "It's just so hard to be sure."
Before leaving for the hospital the next morning, René wrote notes to her children, Cole and Casey, and assured them that she would be okay…but even she didn't know what to expect.
"I have no idea what tomorrow morning's going to be like," she said on the way to the hospital. "I would like to think that there's going to be this immediate sense of relief, in terms of I don't have to worry about ever being diagnosed with breast cancer."
What she did know was that she couldn't continue to live in fear. "My gut tells me I've had enough," she said. "I can't keep doing this to my family. I can't keep doing this to myself."
After René and her husband, Buff, arrived at Memorial Sloan-Kettering Cancer Center in New York City, reality set in. One hour before surgery, René's emotions came pouring out. Through her tears, she asked Buff if she was making the right decision. "I was fine until [the doctor] said we were ready to go to surgery, and then I got scared," she said. "It's just so hard to be sure."
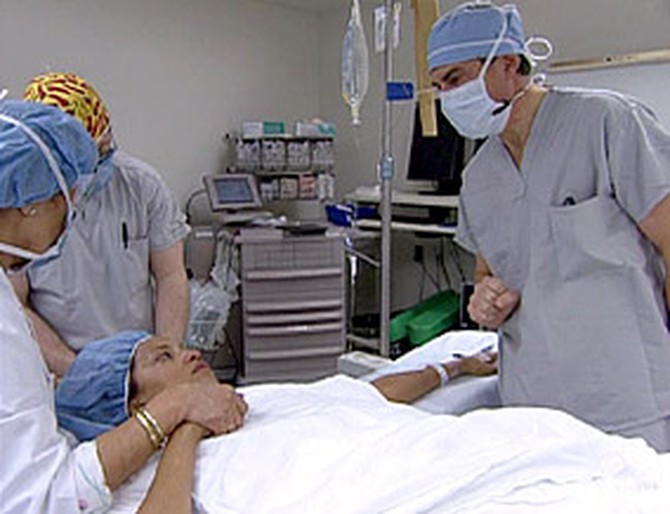
René says she was scared up until the moment she laid her head on the operating table. Then, a team of doctors stepped in to put an end to years of biopsies, lumpectomies and sleepless nights.
To perform the complicated procedure, two doctors with different skill sets had to scrub in. First, Dr. Virgilio Sacchini, a breast surgeon, spent three hours removing all the breast tissue, which can extend under the armpit, under the collarbone and into the abdomen.
Then, Dr. Joseph Disa, a plastic surgeon, inserted temporary breast implants, also known as "tissue expanders." These implants are gradually filled with saline solution until the patient is comfortable with the size and shape of her new breasts.
When René woke up after her surgery, she says she immediately noticed her new additions. "[I had] 360 cc of saline per breast, which felt roughly like two 500-pound gorillas sitting on my chest," she says.
Since her surgery, René has reduced her breast size to a B cup, a full cup size smaller than she once was. "I'm very happy," she says. "I call them my teenaged breasts."
To perform the complicated procedure, two doctors with different skill sets had to scrub in. First, Dr. Virgilio Sacchini, a breast surgeon, spent three hours removing all the breast tissue, which can extend under the armpit, under the collarbone and into the abdomen.
Then, Dr. Joseph Disa, a plastic surgeon, inserted temporary breast implants, also known as "tissue expanders." These implants are gradually filled with saline solution until the patient is comfortable with the size and shape of her new breasts.
When René woke up after her surgery, she says she immediately noticed her new additions. "[I had] 360 cc of saline per breast, which felt roughly like two 500-pound gorillas sitting on my chest," she says.
Since her surgery, René has reduced her breast size to a B cup, a full cup size smaller than she once was. "I'm very happy," she says. "I call them my teenaged breasts."

René came away from her surgery with two small scars and a new lease on life. "I sleep better now than I have I think in five years," she says. "I feel lighter. I'm happy."
Before having a double mastectomy, René had a 40 percent chance of developing breast cancer. Now, the risk has been drastically reduced to 2 percent!
Although she'll never have to have another mammogram or biopsy, René says she'll continue to see a doctor because there's a chance she could develop cancer in her nipple or the areola.
In her book, Good-Enough Mother, René discusses her family life and life-changing choice. She says she hopes that her story will inspire women struggling with the same decision to do what's best for them.
"In all the work that I've done on the Early Show and as a local news anchor, I was always about educating and empowering women," she says. "I really wanted women to know that they had a choice. I made a choice—albeit, not the choice for everyone. But it was the choice for me."
Before having a double mastectomy, René had a 40 percent chance of developing breast cancer. Now, the risk has been drastically reduced to 2 percent!
Although she'll never have to have another mammogram or biopsy, René says she'll continue to see a doctor because there's a chance she could develop cancer in her nipple or the areola.
In her book, Good-Enough Mother, René discusses her family life and life-changing choice. She says she hopes that her story will inspire women struggling with the same decision to do what's best for them.
"In all the work that I've done on the Early Show and as a local news anchor, I was always about educating and empowering women," she says. "I really wanted women to know that they had a choice. I made a choice—albeit, not the choice for everyone. But it was the choice for me."

Dr. Marie Savard, a specialist in internal medicine and author of the book How to Save Your Own Life, says there are women like René who don't know that they are at risk for developing breast cancer.
According to Dr. Savard, there are a few simple medical tests that can help you determine your risk factor. First, Dr. Savard says every woman with a high risk should ask her doctor for a genetic test called BRCA1 or BRCA2, which determines whether you've inherited the gene that causes breast cancer. Eighty to 85 percent of women who test positive will develop some kind of breast cancer.
Though René did not have the gene, her family history was cause for concern. Dr. Savard says that if one or more of your family members have had breast cancer, you should consider genetic counseling. "There are specialists who really help you go through your family tree and understand what your risks are," she says. "Then, [they] help you make the decision about this prophylactic surgery."
Women of Ashkenazi or Eastern European Jewish descent are also at greater risk, Dr. Savard says, and should be tested to see if they've inherited the gene. René says the test costs $3,000, but it was worth it. "It was that important to me to know," she says.
According to Dr. Savard, there are a few simple medical tests that can help you determine your risk factor. First, Dr. Savard says every woman with a high risk should ask her doctor for a genetic test called BRCA1 or BRCA2, which determines whether you've inherited the gene that causes breast cancer. Eighty to 85 percent of women who test positive will develop some kind of breast cancer.
Though René did not have the gene, her family history was cause for concern. Dr. Savard says that if one or more of your family members have had breast cancer, you should consider genetic counseling. "There are specialists who really help you go through your family tree and understand what your risks are," she says. "Then, [they] help you make the decision about this prophylactic surgery."
Women of Ashkenazi or Eastern European Jewish descent are also at greater risk, Dr. Savard says, and should be tested to see if they've inherited the gene. René says the test costs $3,000, but it was worth it. "It was that important to me to know," she says.

The decision to undergo testing is just the first step. Once you find out that you have the breast cancer gene or other risk factors, it's time to take action.
Some women choose medication and other treatment options, while others—like René—choose to have a mastectomy, which has stirred up controversy in the medical community.
Dr. Savard says that some doctors don't recommend the elective surgery, because it's a risky procedure and there's no guarantee that every breast cell is removed. Other medical professionals are worried that women will feel pressure to make this decision when a mere 2 to 3 percent should have to consider it.
Over the years, Dr. Savard says words like "radical" and "mutilation" have also been used to describe the surgery, creating a stigma. "Doctors have made women feel like it's a kind of mutilating surgery, but the bottom line is we have plastic surgery for all sorts of things and nobody questions that," she says. "How could you really question a woman's decision to save her life?"
Some women choose medication and other treatment options, while others—like René—choose to have a mastectomy, which has stirred up controversy in the medical community.
Dr. Savard says that some doctors don't recommend the elective surgery, because it's a risky procedure and there's no guarantee that every breast cell is removed. Other medical professionals are worried that women will feel pressure to make this decision when a mere 2 to 3 percent should have to consider it.
Over the years, Dr. Savard says words like "radical" and "mutilation" have also been used to describe the surgery, creating a stigma. "Doctors have made women feel like it's a kind of mutilating surgery, but the bottom line is we have plastic surgery for all sorts of things and nobody questions that," she says. "How could you really question a woman's decision to save her life?"

Eighty percent of women will contract the human papillomavirus—more commonly known as HPV—in their lifetime. This sexually transmitted virus can lead to cervical cancer…so why is it stirring up so much controversy?
Doctors say a new vaccine that's on the market can prevent HPV, but the sooner you get the treatment, the better. In fact, many recommend that girls as young as 9 years old should be vaccinated, which is troubling to parents who believe that their children are too young to learn about STDs.
Dr. Savard says parents should educate themselves about the disease before making any decisions. The virus, which spreads through skin-to-skin sexual contact, can cause genital warts; but oftentimes, symptoms take weeks, months or even years to appear. In some cases, someone with HPV may never exhibit symptoms—until cancer cells form. A simple medical test can determine whether you're currently living with this common virus.
Most immune systems can fight off the dangerous strains of this virus on their own, but some people's bodies are unable to prevent it from causing major medical issues, including cancer. Dr. Savard says if every woman has three doses of the vaccine before they've been exposed to the virus, no woman will ever die from cervical cancer again.
Doctors say a new vaccine that's on the market can prevent HPV, but the sooner you get the treatment, the better. In fact, many recommend that girls as young as 9 years old should be vaccinated, which is troubling to parents who believe that their children are too young to learn about STDs.
Dr. Savard says parents should educate themselves about the disease before making any decisions. The virus, which spreads through skin-to-skin sexual contact, can cause genital warts; but oftentimes, symptoms take weeks, months or even years to appear. In some cases, someone with HPV may never exhibit symptoms—until cancer cells form. A simple medical test can determine whether you're currently living with this common virus.
Most immune systems can fight off the dangerous strains of this virus on their own, but some people's bodies are unable to prevent it from causing major medical issues, including cancer. Dr. Savard says if every woman has three doses of the vaccine before they've been exposed to the virus, no woman will ever die from cervical cancer again.

Texas Governor Rick Perry has made headlines for issuing an executive order requiring all girls ages 11 and 12 to receive the HPV vaccine before they can enter the sixth grade. This decision has some parents in an uproar over being told how to handle their children's healthcare.
Dr. Savard says it's important for parents to know the facts and protect their children's health. But the mandate could be saving lives, she says. Since the vaccine is so expensive, Dr. Savard believes a mandate may be necessary to help lower prices to make it affordable for all young women.
"It's the underserved, the unprivileged girls in this country who are more likely to die of cervical cancer, [and not be able to] get the pap test in the first place," Dr. Savard says. "That's where the vaccination can make a huge difference. Without a mandate, it's just not going to happen."
Dr. Savard says it's important for parents to know the facts and protect their children's health. But the mandate could be saving lives, she says. Since the vaccine is so expensive, Dr. Savard believes a mandate may be necessary to help lower prices to make it affordable for all young women.
"It's the underserved, the unprivileged girls in this country who are more likely to die of cervical cancer, [and not be able to] get the pap test in the first place," Dr. Savard says. "That's where the vaccination can make a huge difference. Without a mandate, it's just not going to happen."

Some parents have expressed concern that vaccinating their children for HPV is almost like giving their young daughters permission to have sex at an early age. Dr. Savard says that parents need to remember that in order for the vaccine to be effective, it needs to be done before they become sexually active.
"The most important thing is to know the science and to know that the earlier and the sooner they get the vaccine before they're sexually active, the better," Dr. Savard says. "And that's questionable when they're going to become sexually active. You don't always know."
Dr. Savard says parents can approach the subject with their kids by saying it is a vaccine to protect against cancer. She also stresses that since it isn't 100 percent effective, parents should emphasize to girls who are sexually active that they can reduce their risk in other ways—such as practicing safe sex and continuing to get pap smears.
"The most important thing is to know the science and to know that the earlier and the sooner they get the vaccine before they're sexually active, the better," Dr. Savard says. "And that's questionable when they're going to become sexually active. You don't always know."
Dr. Savard says parents can approach the subject with their kids by saying it is a vaccine to protect against cancer. She also stresses that since it isn't 100 percent effective, parents should emphasize to girls who are sexually active that they can reduce their risk in other ways—such as practicing safe sex and continuing to get pap smears.
Published 03/29/2007

