10 Superhero Nurses Making a Big Difference
They tend to us, calm us, and ease our pain—even when it means jumping into a chopper, braving a line of protesters, or scolding a lawmaker or two. Meet ten people who prove that caring is a calling.

Photo: Clay Cook
The Right Track: Whitney Nash and Sara Robertson
Every May, thousands of spectators swan through the stands at the Kentucky Derby, wearing floppy hats and drinking mint juleps. Meanwhile, in the barn area, sweat trickling from under their baseball caps, the "backside workers" muck the stables and walk, bathe, and rub down the horses. These mostly Latino laborers, who typically arrive in Louisville on temporary work visas, are up at 4 a.m. six days a week to keep the $4 billion Kentucky racing economy galloping along.
The laborers, most of whom lack health insurance and can ill afford to miss a day's pay, have been known to work through crippling pneumonia. Marina, a 35-year-old horse walker from Guatemala, once spent weeks ignoring near-blinding headaches. Then she stumbled upon a health fair at which free blood-sugar screenings were being offered by the Kentucky Racing Health Services Center—a clinic providing medical care for track workers for a $5 co-pay. Marina made an appointment for the following week.
The center, established in 2005 by the Kentucky Racing Health and Welfare Fund, was intended to be a walk-in clinic dispensing first aid and antibiotics. But founding director Whitney Nash, PhD, a nurse practitioner from the fund's partner, the University of Louisville School of Nursing, soon learned that many of the laborers had never been to a doctor; she'd do work-ups that revealed chronic issues the clinic was unequipped to handle. Nash, along with nurse practitioner Sara Robertson, wanted to do more for the patients. As Robertson says, "You can't treat a UTI without treating the diabetes causing it."
Over several years, the duo grew the clinic to furnish ongoing care for diabetes, hypertension, and allergies, and offer Pap smears and wellness exams. To encourage workers to come in at the first sign of a problem, Nash and Robertson became a two-woman PR campaign. They printed fliers that said, "Cuando estás enferma, podemos ayudarte. When you are sick, we can help you." They published health articles in the laborers' newspaper and enlisted the track's chaplain to spread the word. And it worked: Mammograms caught breast cancer; patients were diagnosed with serious but manageable heart problems. Says Robertson, "People are still alive because they were screened."
Marina is one of them. At her first visit, she was diagnosed with diabetes and taught to manage it with insulin; at her second, she discovered she was pregnant; in her eighth month, Robertson found she had preeclampsia and sent her straight to the hospital, likely saving Marina's—and her baby's—life.
Today the racetrack clinic is a full-service medical center booking 1,400 office visits every year. Patients can get same-day appointments three days a week; nurses are available for phone consultation daily. Diabetes and psychiatric prescriptions can be filled months in advance for workers who leave town to follow the racing circuit. They can also get counseling for depression, common among laborers who are painfully separated from home and family.
Other states have taken notice: Robertson has consulted with California activists about setting up clinics for agricultural laborers. "Healthy workers, healthy industry," Nash says. "It's a win for everybody."
—Cara Tabachnick
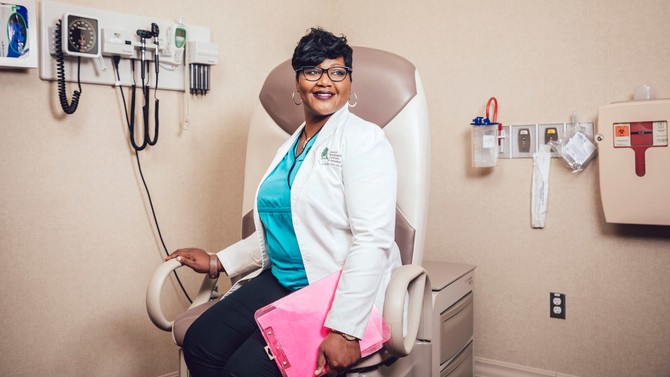
Photo: Audra Melton
Sky's the Limit: Lakisha Henderson
The cancer patient—call her Jane—weakly squeezed Lakisha Henderson's hand. For a grueling month, Henderson had been Jane's nurse at Cancer Treatment Centers of America's (CTCA) Newnan, Georgia, facility, and her care team was discussing next steps. Jane desperately needed a crucial stem cell procedure and would have to fly to CTCA's Philadelphia hospital to get it. "The only way I'm going," she said, "is if Lakisha goes, too."
Henderson is famous around the hospital for going above and beyond. She's visited families at home to console them after the death of a loved one; she sings gospel songs to comfort patients ("Be Ye Also Ready" is a popular request).
However, she'd never gone so literally above, so far beyond as to board an airplane for a patient. As all her coworkers well knew, she was utterly, morbidly afraid of flying.
So what did she say to Jane's proposal? "Let's go."
For days before her trip, Henderson could barely eat or sleep. But every time she wavered, she thought of Jane. "People don't come into the hospital to die, they come in to fight," Henderson says. "And we get right on board and fight with them."
On the dreaded day, Henderson took many deep breaths and an Ativan, then spent the entire flight praying. As soon as she landed, she hurried on wobbly legs to meet Jane at the hospital, where she served as her rock for two days.
Three years later, Jane's cancer is under control. She and Henderson still exchange news about their kids or another clear scan. "Sometimes patients need you to be a sister, a friend, or a mother," Henderson says. "As nurses, we reinvent ourselves every day."
—Kate Rockwood
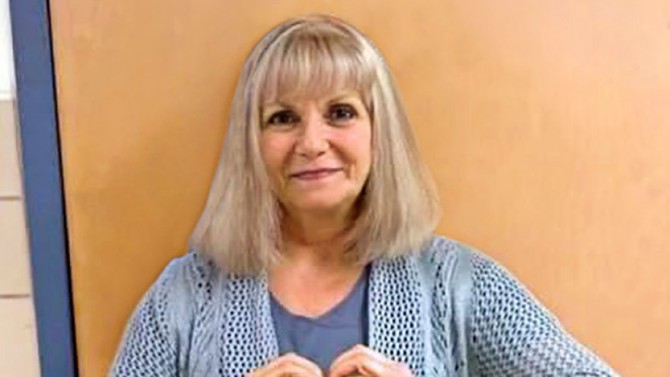
Photo: Courtesy of Patti Butler
Reading the Signs: Patti Butler
The boy arrived for his first full day of kindergarten with gray skin, dark circles under his eyes, and aching legs. The school nurse called his mother, who assumed growing pains and a cold. Nurse Patti wasn't having it: "Those symptoms screamed blood disorder." She convinced his mother to take him to a pediatrician and then a hospital, where he was diagnosed with leukemia. Happy ending: The now 7-year-old is in remission.
Then there was the sixth grader who hit her head at recess. No obvious injuries, but Nurse Patti saw bleeding deep in her ear, a sign of a fractured skull. She called an ambulance but couldn't reach the parents, so she sprinted three blocks to their home. Another full recovery.
Also: the student who started fainting in class. Nurse Patti urged his parents to see their pediatrician, who waved them off. Patti persisted, and a specialist diagnosed the boy with a rare but treatable heart condition.
Nurse Patti is Patti Butler, and for nearly two decades, she's cared for the children of Zane North Elementary School in Collingswood, New Jersey.
Kids today face health issues from autism to obesity; one in four has a chronic condition like asthma or diabetes. Yet because of nationwide budget cuts, less than 40 percent of schools employed a full-time nurse in 2016.
"She goes out of her way for people all the time," says Taylor Catling, the student who fractured her skull. "I remember leaving the hospital and thinking, I want to be like Nurse Patti." And maybe she will: Catling, now 26, was recently accepted to nursing school.
—Leslie Goldman

Photo: Ackerman + Gruber
Being There: Sarah Haeder
Red River Women's Clinic is North Dakota's only abortion facility. Every Wednesday—the day the procedure is performed—a dozen or so demonstrators are already huddled around the building when it opens; by early afternoon, up to 100 people might be brandishing signs: Pray to end abortion. Adoption: the gift of life and love. Women do regret abortion.
By the time a patient makes it past the protesters, she's already endured what's likely been a long drive (North Dakota covers more than 69,000 square miles); a state-required counseling session telling her that abortion will "terminate the life of a whole, separate, unique, living human being"; and a mandatory 24-hour waiting period before going ahead with the procedure. But there's an antidote to her mounting anxiety: kind, steadfast Sarah Haeder, a nurse whose gentle voice some patients recognize from the phone (when she explained the state's rules and reassured them that yes, the clinic would still be open when they arrived, and yes, abortion would still be legal in North Dakota). A hug, a smile, the absence of judgment—Haeder offers exactly what's needed.
The demonstrators tell her, "I know your mother didn't raise you to do this work." And they're right. Growing up, Haeder's parents, both devout Christians, planned family vacations around protesting abortion clinics. When she started college, one of the posters on her wall said every third baby dies from choice.
But after Haeder took a women's studies class, her beliefs began to shift. "I wondered if we were really doing the right thing, " she says. In her early 20s, she supported a close friend through an abortion. When she was 26 and in a new relationship, she became pregnant herself and, after intense soul-searching, decided an abortion was best.
She made an appointment at Red River, which she remembered marching in front of as a girl. The care she received was so compassionate that six months later, she quit her marketing and web design job and applied to join the staff as a patient educator. She counseled women about contraception, female anatomy, what happens during an abortion—and listened to them talk about their decision. And when even becoming clinic manager still didn't seem like contribution enough, she enrolled in nursing school.
Haeder's parents were surprisingly supportive when she told them about her career switch—but they never want to hear about it again. An aunt and two uncles found out the day they were protesting outside the clinic and she squeezed past them. Her extended family no longer shows up at Red River, but neither do they speak to her anymore.
The estrangement hurts. And yet it also fuels Haeder's commitment to reproductive rights. "I need to be there to help other women—especially those who had an upbringing like mine," she says. "If I don't, who will?"
—Amanda Arnold

Photo: Sam Comen
Janel Perez: Taking It to the Streets
Janel Perez doesn't do scrubs. Out on L.A.'s sidewalks, the nurse practitioner opts for discount-store jeans and New Balance sneakers to better blend in among the homeless veterans she tends. Her bag of tricks is a canvas backpack that's like a portable clinic, with a blood pressure cuff, needles, stethoscope, thermometer, bandages, and syringes filled with vaccines for influenza and hep A.
Last year there were more than 40,000 homeless veterans in the U.S., 29 percent of them living in California. In 2011, Perez helped launch a mobile medical team to scour L.A. for these vets and offer them healthcare and a place to live. That pilot program has evolved into a partnership between the U.S. Department of Housing and Urban Development and Veterans Affairs Supportive Housing that serves 6,000 veterans per year, providing checkups, first aid, mental health counseling, and social services, sometimes right there under the freeway.
Many homeless vets wrestle with mental illness and substance abuse, and have developed PTSD from military service or the violence of the streets. They're suspicious of anyone telling them what to do. When Perez first encounters a potential patient, she simply says she's there to help: "We're not asking them to change or get sober first." If they're not interested in talking, she'll come back another day, maybe with a sandwich, and keep checking in every week or so. With the most distrustful vets, months might pass before they're comfortable enough to even let her take their blood pressure.
Perez draws on an endless supply of patience. That's how she won over one air force veteran in his 70s who had lived on the streets for more than two decades. With a lot of nudging, the team was able to persuade him to move into housing, but he refused anything beyond a roof over his head—no furniture, no electricity, no medical care for his schizophrenia. Once a week, Perez would visit him at home, where they'd sit on the floor and chat for an hour about his time stationed in Morocco in the 1960s and his delusions that he was a warrior out to save Santa Monica from destruction.
After four visits, Perez felt emboldened to bring up the E word: "So how about we turn on the electricity?" There was a pause. "Okay," the man said. And then: okay to a bed, to a table, to psychiatric treatment. "To see him now on the medication he needs, going to the grocery store and library, communicating with his sister," says Perez, "shows me we made a huge difference in his life. All those hours of listening were worth it."
—Rachel Rabkin Peachman

Photo: Craig Takihashi/City of Hope
Walking the Walk: Pamela McTague
Monday, you're fine. Tuesday, you find a lump. Wednesday, you leave an oncologist's office thinking you're dying—or will be if you don't subject yourself to the ravages of chemo or surgery. And all the while you can't quite believe it's real. "Many breast cancer patients are like, 'But I don't feel sick!'" says Pamela McTague, a clinical research nurse at City of Hope in Duarte, California.
McTague meets patients after their diagnosis, when they're reeling. She shepherds them through clinical trials, explaining the process and procedures, like radioactive-isotope injections, and monitoring their prognosis. Beyond the hours they're together at the hospital, she maintains an ongoing relationship with her charges, checking in at three months, six months, a year, even five years.
But what really makes McTague a godsend to her patients is the perspective she brings and the hope she embodies. That's because she herself was diagnosed with cancer in both breasts in October 2016, then had a lumpectomy, radiation, and plastic surgery. She credits her cancer with making her better able to prepare patients for the treatment aftermath. "I get what it's like to see yourself in the mirror after surgery," she says.
Even though she didn't have chemo, McTague knows how it changes patients' appearance, and she never wants them to feel self-conscious. So as she talks with them before their procedures (about their family, what's important to them), she pays close attention to each patient's face. "When I see them at follow-up appointments, I want to be able to say, 'Oh, I know those beautiful eyes, that nice smile. You look great.'"
—Corrie Pikul

Photo: Stacy Goldberg
Safe Passage: Kevin Steurer
The call seemed routine: Pick up a toddler with an enlarged heart and bring her back to the pediatric ICU at WVU Medicine Children's Hospital in Morgantown, West Virginia. Kevin Steurer's team jumped into an ambulance and sped two hours into the Appalachian Mountains. When they arrived at the ER of the little girl's local medical center, Steurer, a pediatric transport nurse, took one look at her ashen skin, half-closed eyes, and labored breathing and knew she might not survive the return drive. He grabbed the phone and called the specialist waiting for them. "We'll lose her if we don't intubate," he said, "but I'm worried even that will be more than she can take."
With the clock ticking, Steurer gave the child a diuretic to reduce the stress on her heart and used nasal tubing to deliver oxygen. Yet they still needed to move quickly, faster than an ambulance could go. He decided to change course: They'd take a helicopter.
The girl's sobbing parents refused to leave her side. But there was no room for them in the aircraft, so Steurer explained exactly what he'd be doing and why, and urged them to drive carefully—their daughter would be in excellent hands. Then he tucked the patient into the ambulance, raced her to a nearby helipad, transferred her to the waiting chopper, and monitored her vital signs while the pilot whisked them to the ICU. The 90 minutes they shaved off the trip likely saved her life.
Last year Steurer transported 72 pediatric and neonatal patients; during one especially busy shift, he escorted five children to safety. Not all rescues are harrowing, but when you're bringing seriously ill and injured kids to the ICU and providing emergency care on the way, the stakes are always high.
Performing chest compressions on a tiny patient in an ambulance careening along a twisting backcountry road? Steurer has done it. Inserting a needle into a child's artery between bouts of turbulence at 4,000 feet? He's done that, too. More recently, he's also spent agonizing hours comforting infants who were born addicted to opioids and are suffering withdrawal.
After three and a half years in the field (and the air), often on call for 24-hour shifts, Steurer is now helping train the next generation of mobile child savers. He tells them three things: (1) Trust your gut, because babies can't describe how they feel. (2) It's okay to be scared—scary things happen. (3) Work as a team. To transport that toddler, Steurer coordinated with the WVU doctor, a respiratory therapist, doctors and nurses at her local hospital, a medical command dispatcher, the ambulance driver, the helicopter pilot, and her parents. And after being in the hospital for seven weeks, she was, thanks in large part to Steurer's efforts, allowed to go home and get back to the business of being a 2-year-old.
—Lambeth Hochwald

Photo: Courtesy of Cathy Kennedy
A Port in the Storm: Cathy Kennedy
When the nurses landed in San Juan, Puerto Rico, after Hurricane Maria hit last fall, they gasped at the destruction. And the rest of the island was in even worse shape: Violent winds had ripped roofs off houses, and mudslides had leveled neighborhoods. After days without fresh water, some people were drinking from contaminated creeks.
"The level of chaos was staggering," says Cathy Kennedy (standing, fourth from right), the leader of a team of 50 nurses from the nonprofit Registered Nurse Response Network who had come to provide emergency medicine. Kennedy was in charge of coordinating healthcare volunteers. From a command center in a San Juan sports arena, she sent nurses to buy bottles of water and haul them via school bus to decimated barrios. She organized teams to distribute tubes of hydrocortisone cream to treat rashes caused by dampness.
Every American needs to see this, thought Kennedy. After two weeks in Puerto Rico, she returned to her job as a neonatal nurse at Kaiser Permanente Medical Center in Roseville, California, and started speaking out about what the nurses had witnessed. At a Washington, D.C., press conference, she joined Minority Leader Nancy Pelosi and Puerto Rican members of Congress to plead for aid; in November, she testified before Congress. And when FEMA suggested ending rations—even though almost a third of the island was still dark—Kennedy sounded off again.
This time, it seems, the government listened. In February, Congress appropriated $16 billion in disaster relief funding. Yet the territory is seeking an estimated $94 billion to rebuild and fortify against future storms, Kennedy notes, "and we need to keep holding the government's feet to the fire." Stay tuned.
—Kate Rockwood

Photo: Justin Ketchem
The Pain Reliever: Maureen Sweeney
It's terrifying enough to give birth when you're surrounded by supportive family. But imagine that you're 17—or 14—and pregnancy has brought you nothing but trouble and shame. And your mom is still so angry with you that when you're in the delivery room and it's time for the epidural that would ease your agony, she says no—to punish you. And there's nothing you can do about it because by law you need the consent of a parent or guardian for your own healthcare.
This scene replayed over and over during the two years Maureen Sweeney worked as a labor and delivery nurse at MetroHealth Medical Center in Cleveland. It devastated Sweeney, who had her own first child at 18, to think that girls who were about to become mothers couldn't request spinal pain meds—which over 60 percent of American women rely on to endure vaginal childbirth. "You never get over seeing someone in pain like that," she says.
One night in 2011, Sweeney spent her shift helping a 15-year-old runaway through an excruciating labor and delivery. There was no guardian to sign for her epidural, let alone hug her afterward. Outraged, Sweeney tracked down the head of anesthesiology to get the full story on this cruel rule. He explained that the hospital wasn't to blame—Ohio was.
When Sweeney's shift ended at 7:30 a.m., she went home and started reading up on policy. She discovered that Ohio's healthcare consent laws required adult permission for pregnant minors to have ultrasounds and tests to check for chromosomal abnormalities, receive prenatal care, elect anesthesia, and undergo nonemergency C-sections—leaving young women at the mercy of a parent or guardian or, in the case of runaways, a state child services worker.
That same morning, Sweeney emailed her state representative, Nickie Antonio, whose daughter she'd played soccer with in high school. Antonio promised to look into the situation and indeed drafted a bill later that year. However, the timing was never quite right to bring the legislation to the floor. "Maureen wouldn't let me forget about it, though," Antonio says. Even as Sweeney earned a master's degree, gave birth to a second child, and advanced her career—she's now an associate medical director of FrontLine Service, which helps people in crisis receive mental health care—she kept reminding Antonio about the teens suffering needlessly in labor and delivery rooms.
Last July, Antonio and fellow Democrat Kristin Boggs introduced a bill to the Ohio Legislature that would allow pregnant minors to consent to their own healthcare and that of their unborn child. In February, Sweeney testified on behalf of the bill to a legislative committee, and Antonio is hopeful it will pass by year's end—a joyful outcome to a long and labor-intensive crusade.
—Carlene Bauer
Published 04/27/2018

